Research & Expertise
The primary focus of the lab is disease-oriented laboratory investigation of clonal myeloid neoplasms, employing a range of genomic technologies as well as classical cellular and molecular biology experimental approaches.
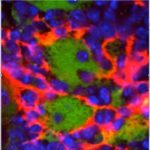
Cellular key drivers of bone marrow fibrosis
Primary myelofibrosis (PMF), an incurable blood cancer, represents the gradual development of bone marrow fibrosis, yet its precise mechanisms remain unclear. Our research identified Gli1+ cells and mesenchymal stromal progenitors as key drivers. Additionally, S100A8/S100A9 emerged as potential markers and therapeutic targets. We are preparing a clinical trial to translate these findings into patient treatments, while our ongoing projects focus on understanding cell activation mechanisms influenced by the bone marrow environment and validating new therapeutic and diagnostic approaches.
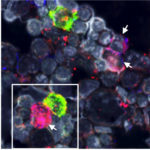
Inflammation and myeloid malignancies
Our recent data identified an unexpected link between haploinsufficiency for genes on Chromosome 5, activation of the innate immune system and myelodysplasia. The activation of the innate immune system was associated with consecutive inflammation in the bone marrow niche and senescence of hematopoietic cells. Our findings underscore a molecular link between the genetic abnormalities in MDS patients, activation of the innate immune system, and ineffective hematopoiesis that characterizes the disease (Schneider et al. Nature 2016).
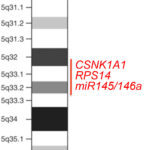
Regulation of the hematopoietic stem cell in del(5q) MDS
Del(5q) myelodysplastic syndrome (MDS) is a clonal disorder of hematopoiesis arising in a hematopoietic stem cell (HSC). In this disease, HSC acquire a deletion of one copy of the long arm of chromosome 5 (i.e. haploinsufficiency of 5q). Our previous studies have shown that the gene dosage effect of haploinsufficiency can be targeted therapeutically, demonstrating an approach for targeting of heterozygous deletions in cancer (Schneider et al. Cancer Cell 2014). In ongoing work we aim to dissect the role of Wnt signaling as an intrinsic mechanism and inflammation as an extrinsic mechanism in the pathogenesis of del(5q) MDS.
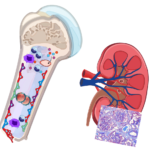
Hematological malignancies and chronic inflammatory diseases
Chronic inflammatory diseases can have a significant effect on normal blood formation. A kidney-bone marrow cross-talk is indisputable as the kidneys filter the blood around 40x/day. However, this cross-talk is far less understood when the functions of either the bone marrow (e.g. through blood cancer) or the kidneys (e.g. chronic kidney disease; CKD) are impaired. In ongoing work, we focus on the vicious and mutual cross-talk between altered hematopoiesis and CKD.
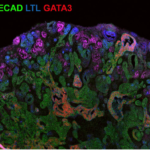
Recapitulating the bone marrow and kidneys in a dish
We have a long-standing interest in recapitulating organs in a dish using human cells or even patient-derived cells for pre-clinical testing. We have collaborations to apply different (smart) materials to provide specific structures for cells to grow, have patient-derived induced pluripotent stem cells (iPS cells) and generated organoids, in particular kidney organoids. We used these kidney organoids to identify the effect of SARS-COV2 on the kidney which correlated well with the situation in patients and helped to uncover a pro-fibrotic effect of SARS-Cov2 on organs.
the lab
We aim to dissect mechanisms in the regulation of the hematopoietic stem cell in myeloid malignancies.
It is a major goal of our lab to identify novel therapeutic targets to specifically eliminate the disease initiating cells and their supporting environment.
In vivo translation studies
Multiplex imaging of bone marrow
GENOMICS & PROTEOMICS
CRISPR/Cas9 gene editing
genetic mouse models
Single-cell technologies
Rebekka is a physician-scientist and received her M.D. degree from RWTH Aachen University, Germany, in 2007 and her Ph.D. degree from Erasmus MC University, the Netherlands, in 2017. Rebekka is the director of the Department for Cell and Tumor Biology at RWTH Aachen, Germany, and a Principal Investigator at Erasmus MC, Netherlands. She was a postdoctoral fellow in Benjamin Ebert’s lab (Brigham and Women’s Hospital, Harvard Medical School, Boston) and focused on the role of genetic haploinsufficiency in hematopoietic stem cell biology and targeted therapy of del(5q) myelodysplastic syndrome.
Her primary focus is disease-oriented laboratory investigation of clonal myeloid neoplasms, employing a range of genomic technologies as well as classical cellular and molecular biology experimental approaches. She has a long-standing interest in dissecting the interaction between hematopoietic cells and the bone marrow niche, in both steady state and myeloid neoplasms. During her fellowship in Pathology with focus on Hematopathology she started to wonder which cells in the bone marrow are responsible for the deposition of fibers in bone marrow fibrosis in myeloproliferative neoplasms. She was particularly frustrated that fibrosis can only be diagnosed when it is already present with standard methods but that it is difficult to predict if a patient will develop fibrosis and that there are no specific anti-fibrotic treatments. This was the starting point for a majority of projects in the lab focusing on understanding fibrosis-driving cells and their activating mechanisms in blood cancer. Additionally, she is very interested in understanding how the hematopoietic stem cell transforms into a malignant cell in blood cancer and how external stimuli (like inflammation and chronic diseases) affect this process.
Her research studies have been considered milestones in the understanding of the del(5q) MDS, were voted as “best in hematology” in 2014 by the American Society of Hematology, she was honored with the Tito Bastianello MDS award of the International MDS foundation 2015, the Innovation Award of German Academic Medicine 2016, the Arthur Pappenheim award of the German Society of Hematology 2016, the Johann Georg Zimmermann Award 2017 (European Cancer Research), the Swammerdam Award of the Dutch Hematology Association in 2019 and the 2022 Gerhard Domagk Award.
Outside the lab, her twins keep her active, she is an outdoors fan, loves cooking, baking, running and (Peloton) cycling.
OUR team in Rotterdam

Stijn fuchs, B.SC
Research technician, lab manager

Aurélie Boeree, B.SC
Research technician

Bella banjanin, MD M.SC
PhD student

Stephani schmitz, m.sc
PhD student

Tesa Klenovšek, M.SC
PhD student

iris Bakker, M.Sc
PhD student

Esra Nur Arslan, M.Sc
PhD student
OUR TEAM IN AACHEN

Anna galyga, m.SC
PhD student

Mohamed saad, M.SC
PhD student

Niklas lutterbach, B.SC
M.SC student

Kristin seré, PHD
Research scientist

Lisa liebenstund, Phd
Veterinarian

katrin götz, M.SC
Research Technician

paul wanek, b.sc
Research technician

carmen schalla
Research technician

susanne schmitz
Research technician

antonio sechi, PHD
Research scientist

Thomas hieronymus, phd
Research scientist
LAB ALUMNI

NIclas flosdorf, M.SC
PhD student, 2019-2023

Katharina reimer, md
Clinician scientist

Ursula Stalmann, MD
Research fellow, 2018-2021

Nils LEimkühler, MD
Research Fellow, 2017-2020

Sergio Martinez-Hoyer, PhD
Postdoctoral research fellow, 2018-2020

Flavia Ribezzo M.Sc.
PhD student
Our recent work
Single-cell analysis of cultured bone marrow stromal cells reveals high similarity to fibroblasts in situ
Mesenchymal stromal cells (MSCs) in bone marrow play key roles in supporting hematopoiesis, impacting diseases and leukemia initiation. Cultured bone marrow-derived stromal cells (cBMSCs) are crucial for simulating hematopoiesis, studying diseases, and finding treatment targets. Comparing cBMSCs’ genetics with in vivo cells shows they differ from fresh MSCs, resembling in vivo fibroblasts, hinting that inhibiting TGFb in labs might maintain a more typical MSC behavior.
Genetic barcoding systematically compares genes in del(5q) MDS and reveals a central role for CSNK1A1 in clonal expansion
Studying how genetic haploinsufficiency affects hematopoietic stem cells in del(5q) myelodysplastic syndrome, our research pinpointed Csnk1a1 as a key player. Csnk1a1 haploinsufficient cells dominated in competition experiments, displaying enhanced self-renewal, proliferation, and resilience under inflammatory stress. This sheds light on how Csnk1a1 deficiency confers a competitive edge to these specific stem cells, shaping disease progression.
Isolation of human bone marrow stromal cells from bone marrow biopsies for single-cell RNA sequencing
This protocol details a method to isolate human bone marrow stromal cells, vital in maintaining stem cell balance and implicated in blood cancers. By combining mechanical and enzymatic methods and FACS sorting, it segregates stromal sub-populations—such as mesenchymal stromal cells, fibroblasts, and Schwann cells—for single-cell RNA sequencing, addressing the challenges of their isolation and preserving their integrity.
Heterogeneous bone-marrow stromal progenitors drive myelofibrosis via a druggable alarmin axis
We sought to map the bone marrow microenvironment in myeloproliferative neoplasms (MPNs) and myelofibrosis (MF) at a single-cell level using murine models and patient samples. Our findings identified specific mesenchymal stromal cell subsets contributing to fibrosis, undergoing distinct functional changes throughout disease stages. We observed the alarmin complex S100A8/S100A9 as a marker of fibrotic progression, both in murine models and patient samples. Tasquinimod, inhibiting S100A8/S100A9 signaling, showed promise in alleviating MPN symptoms and fibrosis in murine models, suggesting it as a potential therapeutic target in MPNs.
Gli1+ Mesenchymal Stromal Cells Are a Key Driver of Bone Marrow Fibrosis and an Important Cellular Therapeutic Target
In our study using murine models, we found that Gli1+ mesenchymal stromal cells (MSCs) originating from specific bone marrow niches drive fibrosis. By genetically tracing these cells and targeting Gli proteins with GANT61, we halted fibrosis progression and rescued bone marrow function. This pathway was also active in human bone marrow fibrosis (BMF), with Gli1 expression correlating with disease severity. Targeting Gli proteins, as shown with GANT61 treatment, holds promise as a potential therapeutic approach for BMF by reducing myofibroblast formation in both murine models and human MSCs.
Rps14 haploinsufficiency causes a block in erythroid differentiation mediated by S100A8 and S100A9
In the context of del(5q) myelodysplastic syndrome (MDS), the loss of RPS14 affects erythropoiesis through a p53-dependent pathway. Mouse models with Rps14 inactivation exhibited erythroid differentiation issues, causing progressive anemia, megakaryocyte problems, and loss of hematopoietic stem cell balance. This defect heightened innate immune signaling, notably via S100a8, contributing to the erythroid malfunction—a connection confirmed as inhibiting S100a8 expression rescued the erythroid differentiation problem caused by Rps14 deficiency.
Nature Medicine 2016

Role of casein kinase 1A1 in the biology and targeted therapy of del(5q) MDS
Our research strongly implicates CSNK1A1 as a key player in del(5q) MDS development. Heterozygous inactivation triggers stem cell expansion and activates β-catenin. Furthermore, targeting casein kinase in Csnk1a1-haploinsufficient cells shows promise in addressing heterozygous deletions in cancer. Additionally, while recurrent mutations were uncommon in the commonly deleted chromosome 5q region, we identified frequent mutations in CSNK1A1 in a subset of del(5q) MDS patients. Overall, these findings highlight CSNK1A1 as a promising therapeutic target for treating del(5q) MDS.
Cancer Cell 2014

LAB ART



LAB NEWS
Excellent oral presentation by Ursula at ASH 2019 and abstract achievement award!!
Successful poster presentation at ASH 2019 in Orlando and abstract achievement award for Nils!!
SCHNEIDER LAB PHOTOS